The pandemic has changed many ways hospitals and health systems operate, but the most notable change is how the patient experience is quickly becoming digital. For some providers, it’s intimidating, but the ones who fully embrace the change and seek the advances that have developed over the years will prosper and ignite patient activation. That involves putting digital health at the forefront of operations.
Providers who want to fully integrate healthcare technology in the patient experience have to be committed to it, but these strategies are key to achieving optimal implementation leading to patient acquisition, loyalty and health outcomes.
Surround the patient experience with digital health tools.
For the longest time, it felt like digital health tools played second fiddle in the patient experience, but that’s not the case today. For most patients, digital patient engagement tools are likely a major part of their experience with providers, if not the entire experience.
For instance, a patient’s healthcare experience may start with a notification to schedule a check-up from their provider’s digital patient engagement and access platform or through SMS/text messaging, email or IVR (Interactive Voice Response). A patient could also message their doctor a simple health question on the digital health platform that leads to a follow-up visit; or, maybe the patient is requesting a prescription refill on the digital health platform. Their entire experience could be digital by scheduling the appointment online, meeting with the doctor virtually through telehealth, filling out an online follow-up survey and paying their bill online.
What’s nice about incorporating numerous digital tools is that patients are in control of their experience, on their own time. This allows physicians, doctors and nurses to focus on tasks that actually align to their job responsibilities. And because all of these touchpoints are tracked digitally, anyone interacting with the patient at any point can get a glimpse of what’s been done and how the provider can help.
Today, it’s hard to imagine not using any patient engagement software within a patient experience. Upfront Healthcare kept this in mind when creating a patient engagement and access platform so that when patients need help getting the care they need when they need it, the system efficiently navigates them in the right direction through a personalized approach.
Use data to route the patient journey.
The patient journey should always begin with the healthcare consumer, but the best way to move it down the line is through data. This can include demographic and socioeconomic data, but it’s hard to find data more compelling than psychographic segmentation data.
A psychographic segmentation model looks at the values, beliefs and ideals of consumers and determines what motivates them based on those feelings. Upfront uses this model to jumpstart patient engagement among healthcare consumers, who are split up into five distinct segments.
Self Achievers: Self Achievers are the most motivated to improve their health. They like to keep track of their progress and work with their doctor to accomplish their health goals.
Balance Seekers: Balance Seekers view their health journey through a wellness lens. Physicians are one of the many resources Balance Seekers use to determine what treatment options work best for them.
Priority Jugglers: Priority Jugglers are always on the go and as a result, don’t put their health first. While they are reactive to their own health, they are proactive for their family members and will do everything to help them get the care they need.
Trustful Responders: Trustful Responders seek the knowledge and expertise of their doctors because they view them as the most credible source for their health. They may not always follow their physician’s advice, but it’s because they’re trying to fit the treatment within their lifestyle.
Willful Endurers: Willful Endurers are the least proactive about their health because they live for the moment. They may not be that unhealthy, but will do what they want whenever they want and will wait until absolutely necessary to go to their doctor.
Through these segments, providers can allow healthcare consumer science to guide the patient journey in an efficient and effective way.
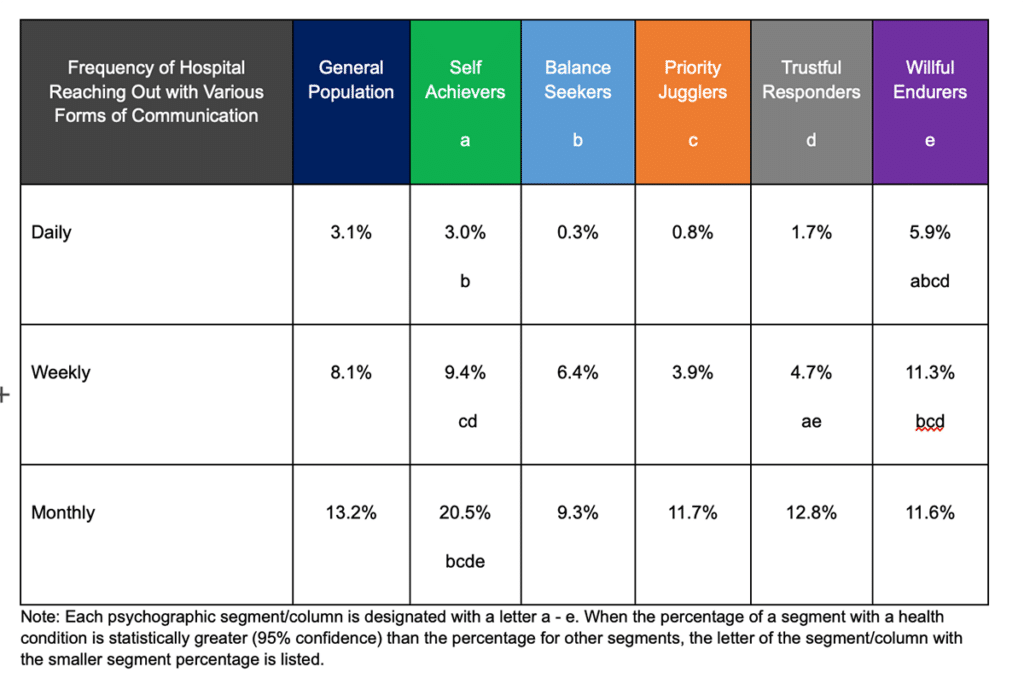
For instance, think about hospital communications. For hospitals trying to reach out to healthcare consumers about a patient payment, Willful Endurers are statistically more likely than any other segment to prefer an automated phone call or a text notification according to Upfront market research. Considering this segment is roughly a third of the general population, providers can reach a large number of people in a compelling way. And 20.5% of Self Achievers, who account for nearly a fifth of healthcare consumers, are statistically more likely than any other segment to prefer monthly communications from hospitals.
Psychographic segmentation can also be used to anticipate possible health problems in the future. Other Upfront market research has found that Balance Seekers are statistically more likely than any other segment to have experienced a stroke in the last 12 months. As a physician, if there’s a Balance Seeker exhibiting heart issues, that could be the indicator that more could develop and to keep an eye on them. The physician could potentially propose a prevention plan with lots of digital resources for the patient to reference, appealing to the research-savvy Balance Seeker.
By having patients do a quick classifier to determine their segment, hospitals and health systems can utilize this vital information to completely transform the way they care for patients and reduce care gaps and unnecessary hospital readmissions.
Seek ways to improve patient activation and outcomes using technology.
For the longest time, hospitals struggled to get patients to follow through on their care plans, but new modes of technology have changed that. It’s imperative that hospitals, when feasible, embrace the newest consumer-preferred, technological advances to revolutionize their patient care.
The pandemic has ignited some of these like telehealth and remote patient monitoring (RPM), which, thanks to new reimbursements, 88% of of providers have either started using or are looking into RPM. Plus, this technology can be life-changing for rural patients who have limited healthcare options nearby.
Another technology, artificial intelligence (AI), has become an invaluable tool to pinpoint diagnosis and treatment plans and assist doctors, clinicians and nurses in a way they never knew they needed. AI is in such high demand that by 2030, the AI market in healthcare is estimated to be valued at $201.3 billion dollars.
Then there are health apps that provide the personalization healthcare consumers are craving and the numerous benefits providers desire like saving on employee labor, relieving precious physician time, reducing operational costs and fostering patient relationships.
At Upfront Healthcare, these digital healthcare innovations illustrate why we founded the Bartosch Institute in 2021. The institute focuses on improving patient activation through best practices in design, product, health communication, data science and research with the goal of improving patient health outcomes. These findings are shared with partners to ensure product and service enhancement while helping them improve their business operations and patient outcomes, but also through thought leadership to drive digital healthcare innovations that improve public health.
As a provider, nothing is more important than improving patient health, and there is no denying that digital healthcare innovations are making a tremendous impact on health outcomes. When hospitals make an effort to integrate digital health into the care experience, it improves the way they operate and the lives of every patient. Learn more about how Upfront’s patient engagement platform can help healthcare systems effortlessly connect with patients.